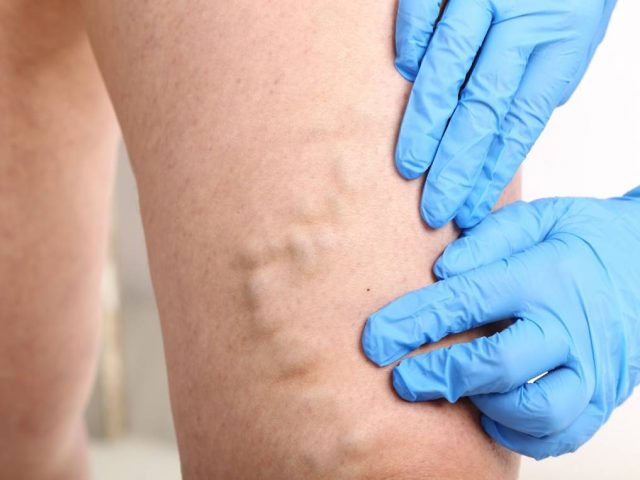
What are varicose veins?
In the human body, a disease called “varicose veins” is often manifested and progresses. This disease is caused by insufficiency of the valve apparatus of the veins and leads to an increase in intravenous pressure and, as a result, varicose dilatation of the vein branches occurs.
Such varicose veins can occur for various reasons and affect different organs of the human body. Most often, the disease affects the veins of the lower limbs, veins of the pelvis, veins of the testes. Separately, it should be noted varicose veins in the presence of malformations (congenital anomalies of development).

Needless to say that in addition to the harm to health, the disease is problematic from an aesthetic point of view. Especially for women.
What populations suffer from varicose veins? What causes development and what are the risk factors?
The most frequent manifestation of varicose veins – varicose veins of the lower extremities and pelvis in women and testicular varicose veins in men. According to statistics, every second woman and every fourth man suffer from this disease throughout their lives. Risk factors that cause varicose veins in women are pregnancy and childbirth, and in men – injuries and active sports, for example, with frequent strikes to the legs while playing football.
Another risk factor is the anatomical structure of the human body. That is a hereditary factor. But in this case we are talking only about the susceptibility to the disease, increasing the likelihood of its occurrence.
Features of the anatomical structure of the body can lead to compression of the veins of the pelvis, left renal or iliac vein and other organs, leading to syndromes that cause massive varicose lesions of the left extremities, spreading to the woman’s groin and labia, and thrombosis. To select the correct treatment strategy, in this case, in addition to the examination of leg veins, it is also necessary to conduct a study of the pelvic veins.
What are the diagnostic methods for varicose veins?
The simplest and most accessible method for diagnosing varicose veins and venous insufficiency of the lower extremities is a study called “Doppler of the lower extremities”. The study is performed to determine valvular insufficiency and is carried out in a standing position, from the groin area and below. At the slightest suspicion of pelvic vein insufficiency, additional studies are needed, such as CT (computed tomography) angiography of the abdomen and pelvis in the arterial and venous phases. If there is suspicion of varicose veins as a result of malformation (congenital anomalies of development), MRI with a contrast agent is necessarily performed.
What are the most modern methods of treatment of varicose veins used?
You can find out how severe your varicose veins are by discussing results of an ultrasound with your physician. Together, you’ll find the best treatment options for your individual case. These may include:
Sclerotherapy: This is a painless saline injection treatment that collapses the vein so that it can then be reabsorbed back into the bloodstream. Navarro says he generally recommends sclerotherapy for small to medium varicose veins. Types of sclerotherapy for varicose vein treatment include:
Laser-Assisted — the least invasive and most advanced
foam sclerotherapy — for larger, more difficult-to-treat veins and ultrasound-guided sclerotherapy — for large, deep veins that once required surgical treatment. The advantage of sclerotherapy is that it can eliminate varicose veins with no pain or downtime.The disadvantage is that the technique may not work for larger, more extensive varicose veins. You may also have to go back for follow-up treatments in order for your veins to completely disappear.
Phlebectomy: Also called vein “stripping,” this is a surgical procedure during which the surgeon makes small cuts near the damaged vein and removes the entire vein. Doctors sometimes do phlebectomy together with other procedures, such as ablation (see below).
The main advantage of phlebectomy is that it’s a permanent treatment because the affected vein is totally removed, But like any surgical procedure, it comes with some risks and requires more recovery time than less invasive methods of varicose vein treatment.
Thermal ablation (also called radiofrequency ablation): Thermal ablation, which has been around for about a decade, involves using laser or radio frequency energy to heat the inside of the vein. This destroys the vein wall, the vein shrinks, and the body absorbs it over time. Thermal ablation tends to work well as a varicose vein treatment, he says, but it can cause a little bruising and discomfort for the first week or so — and because we heat the vein to 200 degrees to destroy it, we need to numb the area around it with an anesthetic, which can cause some discomfort as well.
Veins usually become less visible within one to two weeks. The procedure requires some local anesthesia, but most people have little pain after the procedure and can return to their normal activities the next day.
Non-thermal ablation: Two similar non-thermal techniques were recently approved by the Food and Drug Administration (FDA). The first, Varithna, which the FDA approved in November 2013, uses a medicated foam. It’s basically the same as thermal ablation, but instead of heat, we use a potent drug that destroys the vein more permanently. The second non-thermal ablation treatment for varicose veins, called the VenaSeal system, which received FDA approval in February 2015, uses a glue to shut off the vein.
So far, these procedures seem to work well for varicose vein treatment, he says. But because they are so new, they aren’t time-tested to see if they keep varicose veins under control long term.

How long does the procedure last? What is the duration of rehabilitation? Is the problem solved forever?
The duration of the procedure for each leg when using thermal methods of ablation (radio and laser ablation of the veins), which do not require deep anesthesia, takes about an hour for each leg. A light mask anesthesia is applied with such calculations so that an hour after the operation the patient can return home. He is advised to walk 7-10 kilometers on the same day. After all, movement is something that does not allow postoperative complications to develop.
Incidentally, the “old” methods of operation under general or epidural anesthesia with vein removal throughout are gone, since staying in the supine state for more than a day is the main cause of deep vein thrombosis and other serious complications.
After such a procedure, the patient is recommended to wear elastic stockings for three to six weeks and the maximum possible mobility from the first day.
Special rehabilitation after these procedures is not required. Rehabilitation in this case is a mobile way of life.
Until the moment when the bruises pass and all visible shovchiki disappear, it should take about two months, so we recommend doing these operations in the autumn or winter period. During this period, wearing stockings is more comfortable, and, of course, by the summer there will be no visible marks on the legs.
Modern methods of treatment can delay the next occurrence of varicose veins for 15-20 years or more. When a relapse occurs, these methods make it possible to repeat the procedure.